Severe acute malnutrition (SAM) is the result of a relatively short period of inadequate nutrition which leads to significant wasting and/or oedema and is often complicated by concurrent infective illness. Children with severe acute malnutrition (SAM) are extremely vulnerable to life-threatening complications and have a high mortality if given inadequate or inappropriate care. They require immediate intensive treatment.
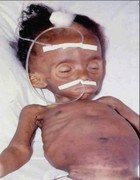
Severe acute malnutrition is:
- Severe wasting, measured by weight-for-height <70% or <-3SD, or mid-upper arm circumference (MUAC) <110mm for children 6 – 59 months, or by clinical signs of severe wasting (marasmus)
- And/or oedema of both feet (kwashiorkor or marasmic kwashiorkor).
Above: Severely wasted child receiving intensive inpatient treatment
Reductive Adaptation
When a child’s intake is insufficient, the needs of the body for energy are met by mobilising tissue reserves of fat and protein from muscle, skin and the gut. Physiological and metabolic changes also take place to conserve energy. These changes take place in an orderly progression called reductive adaptation.
Through reductive adaptation, energy is conserved by:
- Reducing physical activity and growth
- Reducing basal metabolism by slowing protein turnover, reducing the functional reserve of organs, slowing the sodium and potassium pumps in cell membranes and reducing their number
- Reducing inflammatory and immune responses
Consequences of Reductive Adaptation
The changes caused by reductive adaptation have important consequences. The functioning of every cell, organ and system is affected. Here are some of the consequences:
- The liver is less able to make glucose and is less able to excrete excess dietary protein and toxins
- The kidneys are less able to excrete excess fluid and sodium
- The heart is smaller and weaker and has a reduced output
- The gut produces less acid, and smaller amounts of enzymes. Villi become flattened and motility is reduced.
- Sodium leaks into cells due to fewer and slower pumps and potassium leaks out of the cells and is lost in urine
- Iron that is liberated from red blood cells is not stored safely and so promotes the growth of pathogens and harmful free radicals
- Muscle mass is reduced, so there is a loss of intracellular nutrients and glucose stores
- The immune system does not give the normal responses to infection
Severely malnourished children are at risk of death from:
- Hypoglycaemia
- Hypothermia
- Cardiac failure
- Infection
Correct treatment of Severe Acute Malnutrition
Severely malnourished children must be treated differently from other children. The consequences of reductive adaptation must be taken into account from the very start of treatment, no matter what other illnesses the child has. Correct treatment protocol for severely malnourished children must be followed, whether treating the child in the community or as an inpatient.
To prevent deaths from the four most common causes do the following:
- Feed the child straightaway with a specially formulated feed (F75) and give frequent feeds day and night to avoid hypoglycaemia
- Keep the child warm day and night
- Control fluid intake carefully. Do not give IV fluids unless the child is in shock.
- Correct electrolyte imbalance. Give extra potassium and magnesium. Restrict sodium: do not use 0.9% saline IV; use oral rehydration solution for malnutrition (ReSoMal); do not add salt to food
- Give all severely malnourished children broad spectrum antibiotics even if there are no signs of infection. Do not give iron until the child is stabilised.
Click here for more information about inpatient management of SAM. Click here for more information about community-based management.
